Fibromyalgia: Can It Be Reversed? Bestselling Author Dr. Steven Gundry Has a Surprising Answer
Learn what’s causing fibromyalgia and discover how you can deal with your symptoms right at home.
What is fibromyalgia?
Fibromyalgia is a chronic condition. People suffering from fibromyalgia typically experience pain and tenderness in the muscles and bones, in addition to constant – and often crippling – fatigue.
Until quite recently, some healthcare professionals even argued that fibromyalgia wasn’t real. That’s likely because this chronic condition has been both historically difficult to diagnose and largely affects women patients (around 80% of patients diagnosed with fibromyalgia are women).
However, research now shows at least 1 in 40 people worldwide (and, according to the CDC, 4 million Americans) suffer from some form of fibromyalgia. And recent studies have helped scientists better understand what fibromyalgia is and where it comes from.
What are the symptoms of fibromyalgia?
Typical symptoms of fibromyalgia include the following:
- Pain in your muscles or bones that feels like a consistent, dull ache
- Musculoskeletal pain in certain regions of the body
- Fatigue (often constant fatigue)
- Trouble sleeping
- Nonrestorative sleep (that is, sleep that doesn’t leave you feeling rested)
- Headaches
- Lack of focus
- Depression and anxiety
Another common symptom of fibromyalgia is so-called “fibro fog.” This refers to a fuzzy feeling that often leads to problems with thinking, memory, and concentration.
How is fibromyalgia diagnosed?
Fibromyalgia has historically been difficult to diagnose. That’s because fibromyalgia does not show up on a test or x-ray. Additionally, its main symptoms – pain and fatigue – are similar to many other common medical conditions.
Rheumatologists – specialists in muscles, bones, and joints – may be able to help diagnose fibromyalgia. They will often perform a physical exam to check for particular sore and tender points. They are looking for widespread pain in 4 out of 5 specific areas of your body.
Additionally, in order to avoid a misdiagnosis, doctors and specialists will often use a process of elimination to diagnose fibromyalgia. This process may take time and could mean seeing several different doctors and specialists as you seek out multiple opinions regarding your condition.
What causes fibromyalgia?
The cause of fibromyalgia is unknown. The cause appears to be a genetic predisposition combined with certain environmental triggers (including viral infection, stress, etc.).
Most previous theories about the cause of fibromyalgia focused on the roles of the brain and nervous system.
For example, one theory suggests that the brain lowers the pain threshold. This means that over time, previously unremarkable sensations become increasingly more painful.
Another theory is the brain and nervous system may overreact to the body’s normal pain signals.
However, while many of these are only theories, scientists do know that having a family member with fibromyalgia increases the risk of developing it.
Is fibromyalgia an autoimmune disease?
New research suggests that fibromyalgia may actually be a type of autoimmune disease. Scientists discovered that many of the symptoms of fibromyalgia are caused by antibodies that increase the activity of pain-sensing nerves throughout the body.
The scientists harvested blood from 44 people with fibromyalgia and injected antibodies from each of them into laboratory mice. The mice injected with these fibromyalgia antibodies became more sensitive to pressure and cold and displayed reduced grip strength in their paws. By contrast, animals injected with antibodies from healthy people were not affected.
Once the antibodies were cleared from their systems – a process lasting a few weeks – the mice fully recovered.
In other words, this new research shows that fibromyalgia is, in fact, a disease of the immune system. This contradicts previous theories that fibromyalgia originates in the brain.
Fibromyalgia and leaky gut – a surprising connection
Additionally, a 2019 study from Canada found significant differences in 19 species of gut bacteria in women with fibromyalgia and abnormal blood levels of two substances released by some of those bacteria.
This study seems to confirm more recent findings that fibromyalgia is linked to the immune system and is therefore a type of autoimmune disease.
That’s because when the wrong molecules or even bacteria get across the border of your gut wall, your immune system kicks into high gear. Normally, this is really important since your immune system can call in “reinforcements” – inflammatory hormones called cytokines.
These cytokines can save your life from a bacterial infection and help you heal when you have an injury.
The problem starts when your immune system starts responding to every little thing – including environmental triggers or food allergies. Think of it like an overactive security alarm system. You’re grateful when it alerts you to the presence of a thief, but you’re annoyed when it goes off every time a fly enters your home.
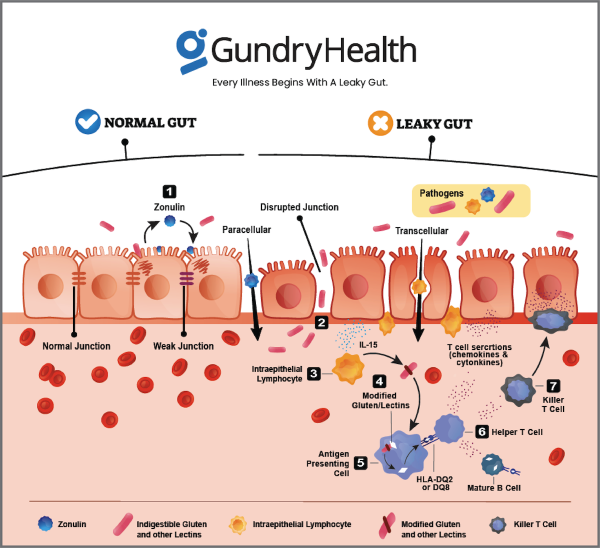
That’s exactly what happens when you have a leaky gut. Your immune system begins responding to everything that gets through your porous gut wall. This leads to chronic inflammation.
Now, what does this all have to do with common autoimmune diseases like arthritis, hypothyroidism, and irritable bowel disease? Well, the zonulin gene sits on a certain chromosome linked to many autoimmune diseases, certain types of cancer, and diseases of the nervous system like multiple sclerosis. In other words, there’s a clear connection between a leaky gut and the formation of autoimmune diseases.
So while genetics and your environment do play a role in whether you develop autoimmune diseases, a leaky gut is the crucial third ingredient. This is why it’s so important to keep your gut wall strong. And unlike your genetics, and often unlike your environment, you can fix a leaky gut.
How to treat fibromyalgia
Previously, most treatments for fibromyalgia included some combination of gentle exercise along with drug and psychological therapies to try and manage pain. However, these treatments have largely proved ineffective for managing fibromyalgia symptoms.
For instance, many fibromyalgia patients are prescribed anti-pain medications. While these pain medications – including over-the-counter options like ibuprofen and naproxen – may help temporarily relieve painful symptoms, they can also contribute to worsening of symptoms.
These two painkillers are a type of drug called a non-steroidal anti-inflammatory – or NSAID. There’s now considerable evidence that NSAIDs can cause significant damage to the lining of the stomach, small intestine, and colon.
Considering the growing evidence suggesting a link between fibromyalgia and the gut microbiome (the bacteria living inside your gut), NSAIDs like ibuprofen and naproxen may make fibromyalgia symptoms worse in the long-term.
Understanding this link between fibromyalgia and the gut is key to treating the disease. It’s why, in his private practice, Dr. Steven Gundry always begins with blood work. He looks for specific markers of inflammation and leaky gut, before asking the patient a battery of questions about symptoms, diet, and lifestyle.
Once he’s made his diagnosis, Dr. Gundry works with his patients to craft a personalized diet and lifestyle routine. This program may also include specific recommendations to help a patient heal her leaky gut.
If you suspect you may have a leaky gut, there are some steps you can take at home right now.
First, eat more prebiotic fiber. Prebiotics are the food your beneficial gut bacteria love to eat. And they’re particularly good for you precisely because you can’t digest them. Prebiotics pass through your stomach and into your gut, where your “good” bacteria can digest them.
Prebiotic-rich vegetables include artichokes, leeks, okra, jicama, broccoli, Jerusalem artichokes, cauliflower, radicchio, and chicory. You can also find prebiotics in mushrooms and some nuts.
Second, you may also want to cut lectin-containing foods from your diets. These include foods like oats, quinoa, brown rice, barley, rye, and whole wheat – along with nightshades like tomatoes, potatoes, and peppers.
However, please keep in mind that nutrition is highly personalized. What’s right for one person may not be right for someone else. So while these recommendations are generalizable, following these suggestions may not solve your leaky gut.
That’s why it’s important to speak with a certified expert who can give you more personalized diet and lifestyle recommendations.